Visual Evoked Potential (VEP)
What is Visual Evoked Potential (VEP)?
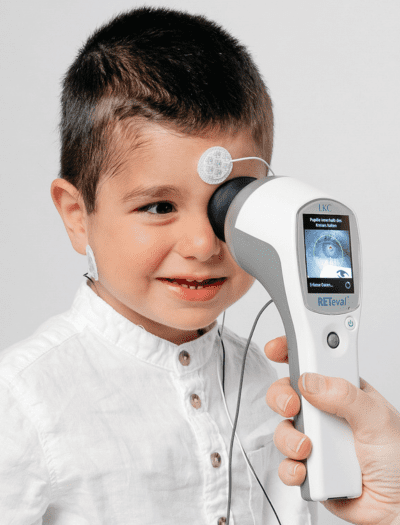
How VEP works
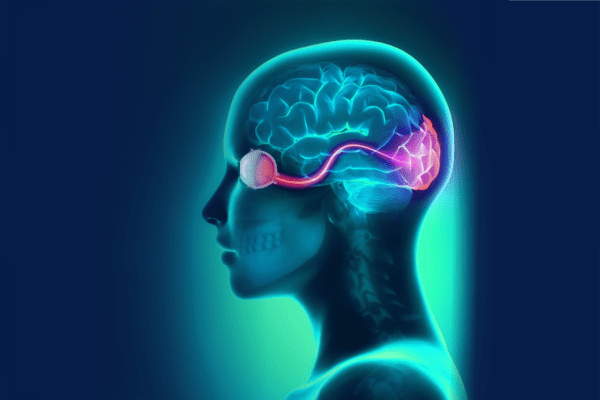
A light stimulus provided by a computer monitor or ganzfeld bowl is received by the retinal cells of the eye. The electric potential travels from the retina to the visual cortex of the brain. Electrodes placed on the occipital lobe record the resulting electrical activity within the visual cortex.
What VEP tells us
Abnormalities in the VEP indicate potential distruptions in the visual pathway. VEP can help to detect the causitive mechanism of visual deficits.
- It is useful as a test of the visual pathway as a whole.
- Normal VEP indicates that visual information is successfully transmitted to the brain’s visual cortex for interpretation.
- Abnormalities may indicate issues with the transmission from the eye to the visual cortex.
VEP testing provides functional and objective data
VEP is a non-invasive measure of the electrophysiological responses of the brain to visual stimuli. VEP testing provides objective and recordable functional information even for non-cooperative, non-verbal, or unconscious patients.
Although imaging technology like MRI continues to advance, VEP is regarded as a valuable tool to help detect occult lesions within the visual pathway, and most especially within the optic nerve.

Why conduct VEP testing?
VEP is an objective test of visual function. Numerous syndromes and anomalies can affect the VEP, including optic neuritis, multiple sclerosis (MS), tumors, traumatic injuries, infections, and toxic agents. Interpretation of the VEP abnormalities can help differentiate between possible types of underlying pathologies.
Clinical Applications of VEP
VEP, as an aid in diagnosis and disease management, is clinically valuable to clinicians in the determination of neurological deficits causing vision issues — even when imaging is unreliable or inconclusive, or when symptoms appear to be subjective only. Likewise, VEP can be used to track functional recovery after an acquired or traumatic neurological event.[44]
VEP testing can therefore be used to assess:
- Misrouting in the optic nerve fibers (e.g. albinism)[43]
- Toxic or nutritional optic nerve dysfunctions[43]
- Optic neuritis suspects (resulting from demyelination e.g. multiple sclerosis)[42]
- Recovery from a range of optic pathway dysfunction[42]
- Cortical blindness due to meningitis or anoxia[42]
VEP testing can also be used to:
- Distinguish between inflammation and other optic neuropathies[42]
- Quantitatively ascertain visual system function and optic pathways due to head trauma[42]
- Help detect orbital tumors compressing the optic pathway[42]
- Monitor for potential optic nerve gliomas in patients with neurofibromatosis[42]
- Monitor cerebral function of patients in operating rooms or intensive care[44]
3 Types of VEP Tests
Different visual stimuli have been designed to produce different types of VEP results. In general, the clinically most used types of VEP testing are pattern-reversal VEP (PVEP or PRVEP), pattern-onset VEP, and flash VEP. Pattern-reversal stimulation is the gold standard for VEP testing, with the most consistent timing and waveform.[45] On the other hand, pattern-onset VEP and flash VEP are more commonly used for patients who cannot fixate, such as infants.
RETeval, VEP Testing Made Simple
More about the RETeval ERG/VEP device
Popular Topics: Make a Difference in Diabetic Retinopathy Care | Glaucoma Evaluation with RETeval PhNR Test | RETeval Device Reference Data | RETeval in Optometry
Case Studies: ERG Demonstrates Stable Function Despite Severe Structural Damage | ERG Supports Treatment Decision in Diabetic Retinopathy | Photopic Negative Response as a Reliable Method for Glaucoma Follow-up in Children | A Tale of Two Patients | Vision Complaints Reflected on ERG | Predictive Value of Combining Diagnostic Technologies| ERG Provides Clarity When Fields and OCT Are Inconclusive| ERG Raises Red Flag, Changing Management Trajectory | ERG Provides Confidence to Monitor or Treat | ERG to Determine Ischemic Status | ERG to Replace FA for CRVO Treatment Decision | Using ERG to Monitor Glaucoma | Routine ERG Use Supports Complex Patient Management | ERG Alters Follow-up Schedule and Education for Patient with Diabetes | Using ERG for Management of Birdshot Chorioretinopathy | Using ERG to Monitor Glaucoma | Comprehensive Pediatric Assessment Using ERG in Challenging Cases | ERG Above and Beyond Retinal Imaging | ERG’s Role in Diabetic Retinopathy Progression Monitoring | ERG-based Risk Assessment in CRVO | ERG Supports Diagnostic Accuracy in a Pediatric Patient
Ebooks: Core Cases from the Clinical Compendium | Modern Fundamentals of Diabetic Retinopathy Management in Optometry | Elevating Patient Care with ERG
Articles: Electroretinography Added to AAO’s Diabetic Retinopathy Preferred Practice Pattern Guidelines | How Comfortable is the RETeval for Patients? |The Use of RETeval ERG/VEP in Pediatric Ophthalmology | How RETeval ERG Has Enhanced My Practice | The Use of RETeval ERG/VEP in Pediatric Ophthalmology | The Ultimate Guide to Diabetic Retinopathy in Primary Eyecare | What Type of Functional Testing Do You Prefer for Patients with Diabetes? | Major Milestone: RETeval Referenced in over 200 Publications | Collaboration to Elevate the Standard of Care for DR | Is ERG Needed if You Have Access to a Good Structural Imaging Device? | A Straightforward Approach to Managing and Supporting Patients with Diabetes | Simplify Grading and Risk Assessment in Diabetic Retinopathy | Simplify Daily Decision-Making with Modern ERG | Objective Functional Testing Needs in Diabetes and Glaucoma | Why Modern ERG is Re-Defining Diabetes Management | Diabetic Retinopathy Management Protocols for Optometry
Videos: RETeval: More Information, Better Decisions | RETeval: Eliminating Confusion in Clinic | RETeval: Function to Rely On | RETeval Handheld ERG: Features & Benefits | RETeval: Enhancing Collaborative Care | Handheld ERG for Primary Eyecare | Advice for Optometric Colleagues about Handheld ERG | Making a Difference in Diabetic Retinopathy Care | Changing the Way We Think About Electrodiagnostics | ERG Testing Made Simple | VEP Testing Made Simple | ERG Waveform | Introduction to Visual Electrophysiology | A Superior DR Progression Risk Assessment with the RETeval Device | Improve Glaucoma Management with the RETeval Handheld ERG Device | Reshaping the Retinal Diagnostic Landscape | New Solutions for Infants with ROP | Using the RETeval in Myopia Research
Webinars: ABCs of ERG | Ready for RETeval | ERG in Action | Blueprint for Functional Assessments | Predicting Vision Loss in a Busy Retina Practice | Objective, Functional Testing for Glaucoma? | Best Management Practices for Diabetic Retinopathy | How the RETeval Device Became a Daily Instrument in my Diagnostic Toolkit
